Please choose a body region on the right for you to pin point the problem area of your body.

Shop by Condition

Shop by Brand
A Hida Hand Health Tool
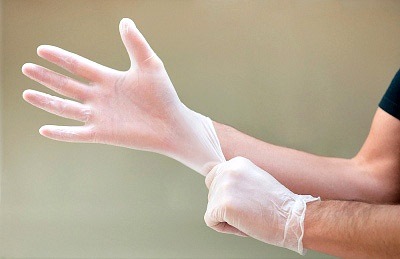
HIV. Hepatitis C. Anthrax. The best way to avoid contact with microorganisms and to avoid widespread contamination among clinicians and patients is to put a barrier between hosts. This means selecting a glove that will provide the tactile sensitivity and strength needed to perform the task at hand while controlling glove associated reactions and exposure to infectious substances. To accomplish this, clinicians need to evaluate the performance and durability of a glove’s base material and consider these factors in conjunction with the level of patient contact, the procedure being performed, and the exposure and infection risks associated with providing care.
BASE MATERIAL:
Gloves can be manufactured from latex, vinyl, nitrile, polyurethane, neoprene, and a host of other materials. Each barrier has its strengths and weaknesses. Latex is flexible, strong, and long lasting, but latex allergies can produce severe reactions. Vinyl gloves can be an alternative to latex, but the barrier can crack, break, or separate when stressed by instruments, fingernails, or stretching. Nitrile is resistant to many chemicals and resistant to punctures and abrasion but tends to be stiffer than latex. Other glove materials can be degraded when exposed to certain chemicals commonly used in patient care setting or when improperly stored.
COMMON PRACTICES:
Glove performance can only be as good as the practices that maintain their integrity. Certain oils, such as Vaseline, can break down latex and should be washed away before glove donning. Fingernails and jewelry can tear or compromise virtually any glove’s performance. Gloves not properly changed between tasks and procedures can spread infectious agents. Glove material can be fatigued by rigorous manipulation. Clinicians must consider activities and practices when selecting their gloves.
POWDER:
Glove powder can absorb latex proteins and other chemicals. As a result, glove powder can become aerosolized during donning and glove removal and provide a vehicle for spreading latex proteins and other substances. Powder can also carry microorganisms, which could contribute to disease. Powder in a wound or surgical site can reduce the effectiveness of the patient’s local immune system making him more vulnerable to infections. Strong consideration should be given to restricting the use of powdered gloves in contagious infection wards, in immune-comprised isolation setting, in neonatal units, and in surgical environments. The National Institute of Occupational Safety and Health (NIOSH) recommends that latex gloves be powder-free, with reduced protein content.
PERFORMANCE
It is essential that gloves have the barrier durability needed to perform the task at hand. Glove durability needs to be considered when contact with infectious materials is expected.
Get $10 off your next order when you sign up to receive our email newsletter.*
Simply enter your email address below!
*Minimum order value of $100. Valid email address to qualify.